Media ID: 55385141
Caption:

Media ID: 55384665
Caption:

Media ID: 55384532
Caption:
Media ID: 55383719
Caption:
Media ID: 55383709
Caption:
Media ID: 55383584
Caption:

Caption:

Caption:
FILE PHOTO: The Nutrition Facts label is seen on a box of Pop Tarts at a store in New York February 27, 2014. REUTERS/Brendan McDermid

Food Trends and Your Heart
Cambridge- The type and amount of fat, carbohydrate, sugar, and salt in our food supply has changed over the years — for better and for worse. Remember when packaged foods emblazoned with the words “fat free” seemed to be everywhere? Then came labels...Caption:
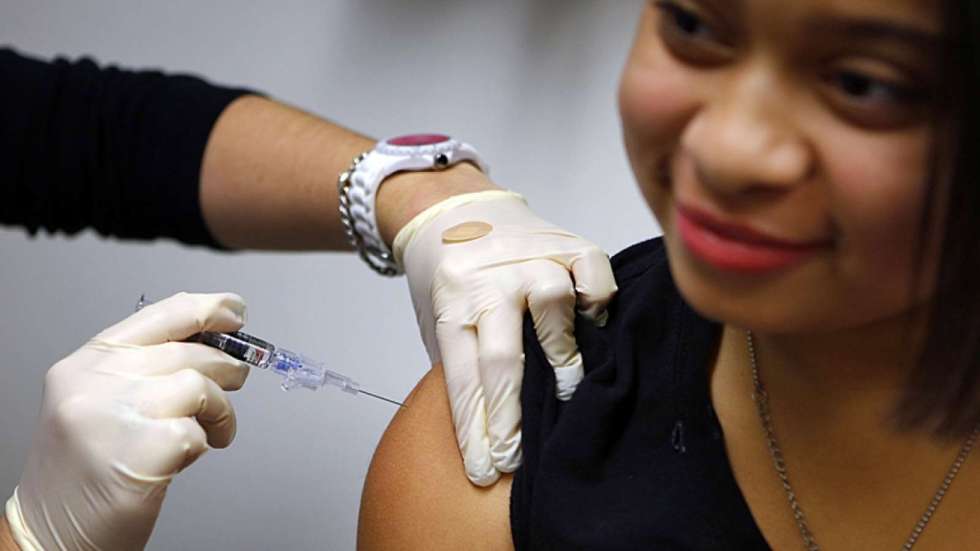
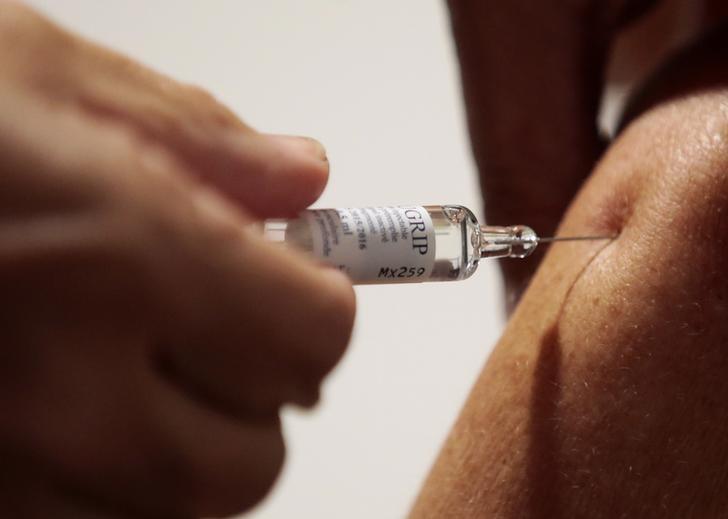
A nurse vaccinates a patient as part of the start of the seasonal influenza vaccination campaign in Nice, southeastern France, October 21, 2015. REUTERS/Eric Gaillard

Oxford University to Test Universal Flu Vaccine in World First
A seasonal flu vaccine that would be the first in the world to fight all types of the virus is to be tested in a two-year clinical trial involving more than 2,000 patients by researchers in Oxford. The so-called universal vaccine was developed by Oxford University’s...Caption:
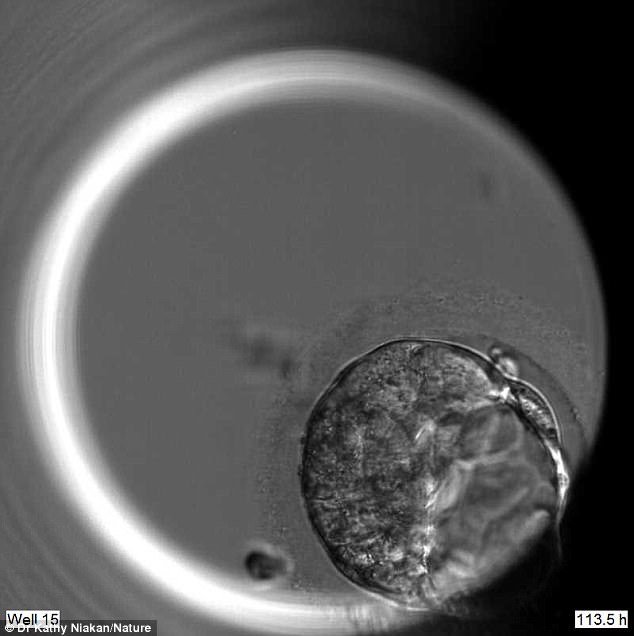
Scientists used the CRISPR-Cas9 system to ‘edit’ growing human embryos to see what would occur when a key gene was removed. Pictured is an edited embryo without OCT4 on the fifth day of development – it does not form a proper blastocyst

Scientists Edit Embryos’ Genes to Study Early Human Development
London- British scientists have used a genome editing tool known as CRISPR/Cas9 to knock out a gene in embryos just a few days old, testing the technique’s ability to decipher key gene functions in early human development. The researchers said their experiments, using...Caption:
Close-up of a model of the human heart

Should You Consider a Coronary Artery Calcium Scan?
If you’re on the fence about whether to take a statin, this test might make sense. Cardiologists constantly seek better ways to predict who will have a heart attack. Among the many potentially helpful options is a coronary artery calcium scan. This test uses a special...Caption:
